Automating Claims and Payment Status Inquiries in Healthcare
Client
Global Manufacturing Leader
Industry
Healthcare
ROI
275
Months
7 months
Use Cases
Customer Support, FAQs, Live agent support
Technologies Used
AI Chatbot, Automation, Contact Center AI

Business Problem
A leading healthcare provider faced mounting inefficiencies in handling claims and payment status inquiries with insurance carriers.
These manual processes significantly impacted operational throughput, staff morale, and the organization’s ability to scale and take on larger client accounts.
Additionally, reliance on voice calls for status updates hindered real-time visibility and created friction in the revenue cycle.
Business Solution
Pronix Inc. implemented a voice-enabled AI automation framework to transform the claims interaction process. The solution eliminated the need for staff to manually call carriers by automating inbound and outbound claim/payment status interactions via intelligent voice systems. It also enabled omnichannel access for real-time status updates across web and mobile touchpoints.
The intelligent automation platform provided seamless handoffs for complex cases, ensuring smooth escalation without data loss. Through contextual workflows and natural language interactions, the client achieved faster turnaround, reduced manual workload, and greater scalability.

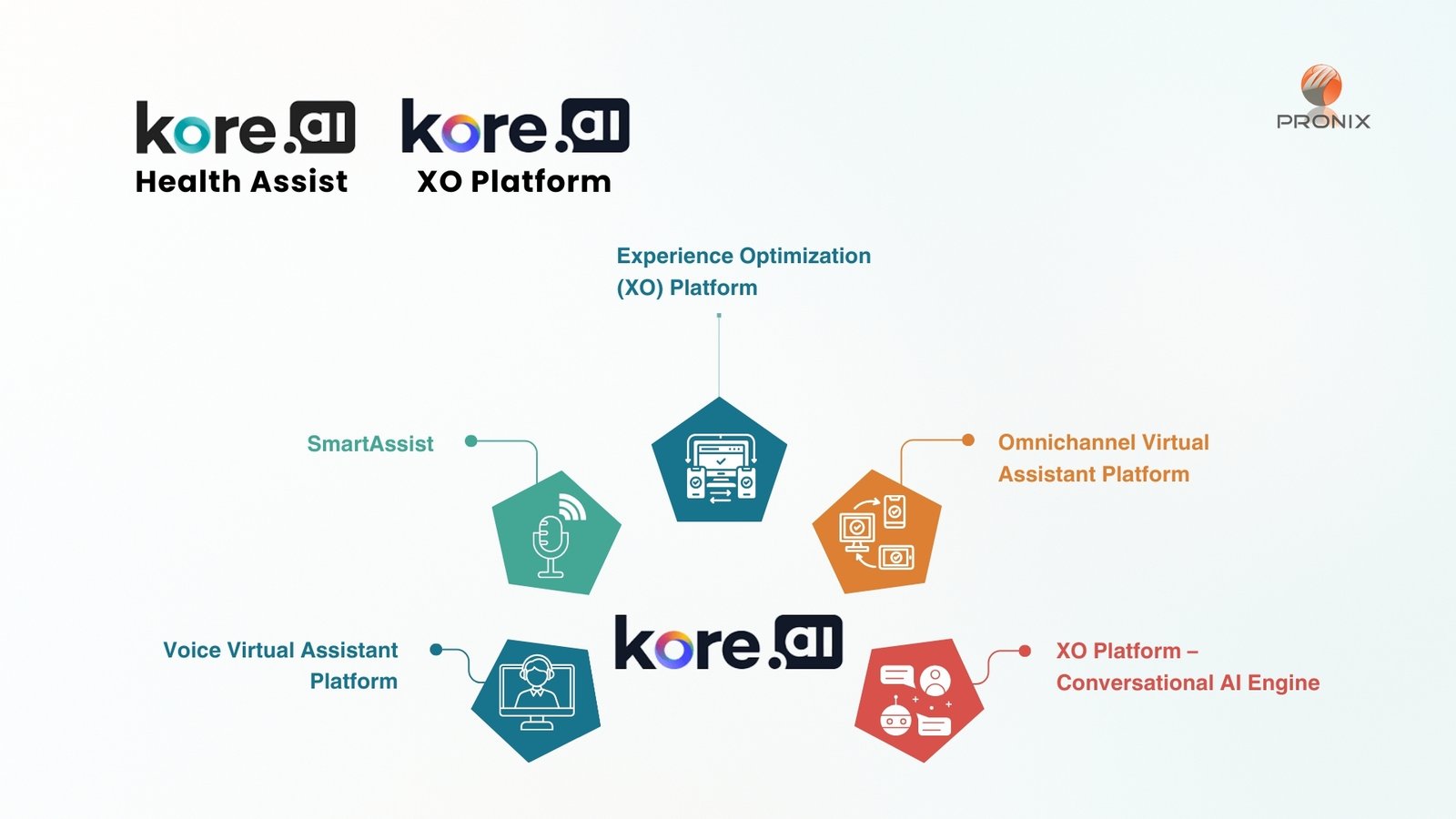
Technologies Used
Technical Solution
- Voice Bots – Automated status checks with insurance carriers via phone calls, reducing wait time and manual intervention.
- Intelligent Virtual Assistants – Understood and responded to inquiries in natural language across voice and chat channels.
- Agent Handoff Framework – Routed complex queries to human agents with complete interaction history for contextual support.
- Omnichannel Integration – Delivered updates to staff and patients via web portals, mobile apps, and email/SMS.
- Backend System Integration – Connected with the client’s claims management and EHR systems for real-time data retrieval and validation.
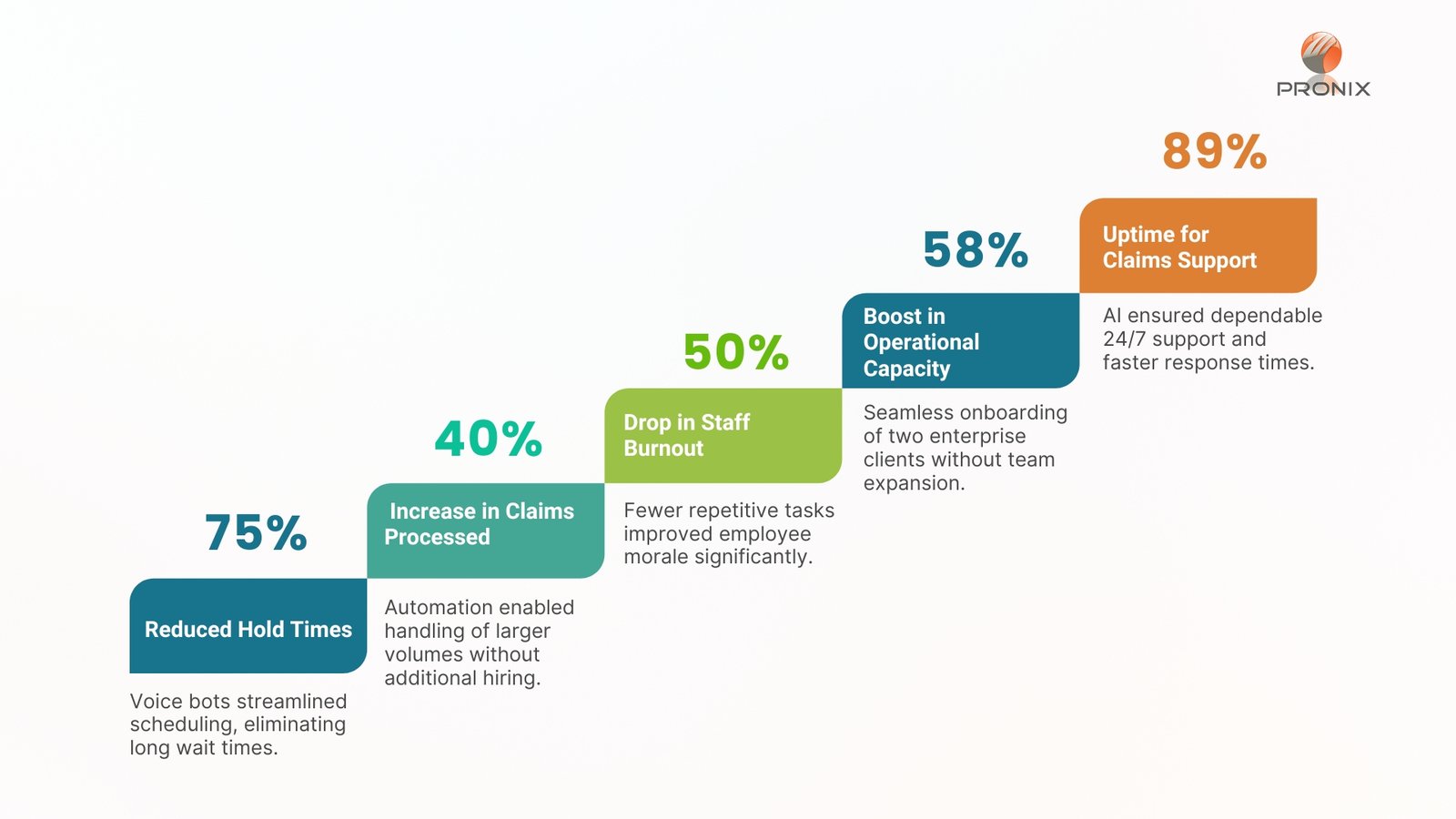
Customer Success Outcomes
OPERATIONAL CAPACITY